Covid-19 has decimated populations and overwhelmed health systems, but the pandemic has also accelerated innovation efforts as dire circumstances increase the urgency of change and the willingness to conduct higher-risk experimentation. Social entrepreneur Michael Seo, who launched a Kenya private health clinic serving vulnerable populations, looks at potential lessons for Asia.
Prenatal clinic in Bihar, India: Women should be involved in all aspects of designing healthcare ventures for women (Credit: Travel Stock / Shutterstock.com)
Infectious diseases are devastatingly egalitarian and the global scope of the pandemic has forged a shared vulnerability that is driving intense efforts to combat Covid-19. In global health, the dual burden of disease refers to health systems dealing with infectious and chronic diseases simultaneously. There is also a dual window of opportunity: to fortify health infrastructure, and to take a systemic approach to investing in healthcare innovation, particularly initiatives led by women.
According to a McKinsey survey, 90 percent of executives believe the Covid-19 pandemic will fundamentally change their businesses, and 85 percent predict lasting changes in customers’ preferences. But openness to change cannot be capitalized upon when a significant pool of innovators and entrepreneurs – women – are not enabled or supported to innovate and scale up ventures.
In October 2020, nearly eight months after the start of the pandemic, a World Health Organization (WHO) study looked at more than 1,000 new or modifications of existing technologies that were developed worldwide to respond to Covid-19. The analysis identified over 120 examples, or about 12.8 percent of the total, that were piloted or adopted in Africa. The response areas included surveillance, contact tracing, community engagement, treatment, laboratory systems, and infection prevention and control.
In 2020, the World Bank Group, the International Monetary Fund (IMF) and their partners mobilized more than US$55 billion in Covid-19 funding to bolster front-line health services, support vulnerable populations and boost deteriorating economies in Africa. Improving global health and gender equality are integral components of the 2030 Agenda for Sustainable Development of the United Nations, or the Sustainable Development Goals (SDGs). Sizeable programs directed at Covid-19 present an unprecedented opportunity to address the gender imbalance of access to opportunity, development and support.
It’s the women in the economy, stupid
Consider the work of the PharmAccess Foundation, an NGO headquartered in Amsterdam, Netherlands, with four country offices across Africa. PharmAccess is led by a female chief executive, and across the organization, half of the global management team are women. PharmAccess’s entrepreneurial approach to address vexing problems in health has resulted in mobile payments platforms such as M-TIBA and CarePay that have reshaped how financial inclusion can be expanded to the unbanked and vulnerable. At the small-and-medium-enterprise level, its Medical Credit Fund provides working capital to growing health businesses.
In Africa, women represent about 70 percent of the health workforce but only 30 percent of science professionals. Meanwhile, the continent has the highest rates of female entrepreneurship, yet according to the African Development Bank, there is a US$42 billion funding disparity between men and women entrepreneurs. (A similar landscape exists in the Asia Pacific. In ASEAN economies, for example, women-owned micro enterprises with adequate financing accounted for just 5-6 percent of the total. For small and medium-sized enterprises, the figures are 12-15 percent and 17-21 percent, respectively.)
In trying to make sense of this inequity, Nicole Spieker, East Africa director and director of quality at PharmAccess, overseeing its innovation agenda, points out that historical and cultural precedence are often antithetical to the needs of identifying and cultivating female innovators. “We know from our work that Kenya has great women leaders, with a rising generation of women leaders. The pandemic has been devastating. There is, however, excitement for the opportunities borne out of great need. Clearly, what the pandemic shows is the irrefutable link between healthcare and economics and economies.”
Initiatives such as the Medical Credit Fund play a critical role for entrepreneurs, providing working capital and bridge financing for African micro, small and medium-sized enterprises (MSMEs). With less access to financing, women entrepreneurs globally, not only Africa and Asia, are more likely to face a liquidity squeeze where they are not able to collect earnings quickly enough to pay expenses. This cash-cycle debt problem can topple “successful” businesses, which might have substantial earnings activity but actually have little cash on hand.
Across the board, a gender lens
Weaknesses in health systems are not uniform across regions and countries or within countries. For example, the United Nations Population Fund (UNFPA) reports that in the Asia-Pacific region, in 2010, for every 100,000 births, 150 women died from complications related to pregnancy and childbirth. Subregional differences were significant: In South Asia, the figure was 220, compared to 150 in Southeast Asia and just 37 in East Asia.
In Africa, the UNFPA reports that only about half of the 123 million women who give birth each year receive antenatal, delivery and newborn care. In developing countries, there are too few properly equipped health facilities for women, and those that do exist rarely provide all of the care that women and babies need.
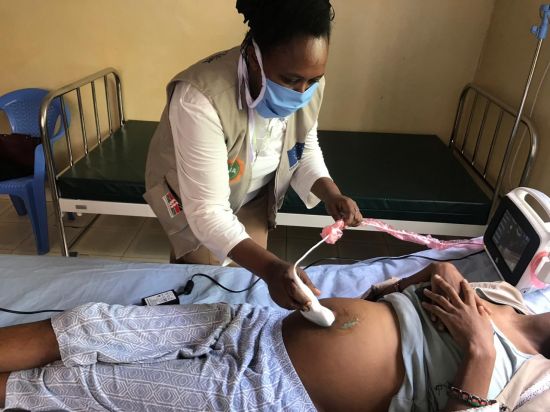
At ReaMedica Healthcare Kenya, which I founded in 2018, a value-based healthcare approach to innovation is predicated on a nurse-midwife-centric services model. The evolution of point-of-care-ultrasound (POCUS) limited obstetric scanning is focused on process improvement based on our mission to address the challenge of equitable access to ultrasound imaging in prenatal care that has proven clinical efficacy.
As most maternal care nurses and midwifes in Kenya are women, the service-design process was explicitly gender conscious. Penina Mulwa, RMH’s director and a female nurse-midwife, co-led the design and implementation, which included focus groups, interviews and surveys that were planned and reviewed by female midwives and nurses. The objective was to create not merely an ultrasound report but one that a nurse or midwife could act on immediately.
In the second half of 2020, RMH began two POCUS pilot programs. The aim of the Lumify project of the PharmAccess Foundation Kenya and the Philips Foundation is to analyze the price elasticity of ultrasound services for different communities through varying health service providers so that access to affordable quality imaging can be expanded sustainably and equitably. In the other initiative, RMH is collaborating with the Murang’a County Department of Health to bring nurse-midwife-managed POCUS to clinics not equipped to provide prenatal imaging.
Challenges for the woman entrepreneur
Often innovation leads to new challenges. Digital health initiatives, for example, are requiring more interaction among health professionals, patients and stakeholders. The increased contact, physically and virtually will require new interpersonal and problem-solving skills. In India and China, McKinsey & Co has estimated that up to 40 million health workers will need to enhance their skill levels to stay viable in the workplace.
Dr Harriet Mwithaga is a Kenya Medical doctor, entrepreneur and the founder of Health Connect, an online matchmaking marketplace for health professionals, health organizations and individuals seeking private medical services. Health professionals register to be available to health organizations as well as individuals seeking trusted qualified service providers The platform launched a beta version in December 2020 and went fully operational at the end of January 2021.
As a physician, Mwithaga is acutely aware of the need to provide safe and reliable health services with the necessary safeguards against Covid-19. Because of the pandemic, many people are afraid to seek care in hospitals and clinics. The Health Connect platform is intended to build trust with patients so that they can receive the services they need in safe settings. It is also aimed at providing flexible staffing to health providers and assure temporary health workers that they will be paid in a timely manner.
Mwithaga is well aware of the challenges that women entrepreneurs face, especially when creating innovative products and services. “Qualifications and talent are only the price of entry,” she explains. “As women entrepreneurs, we constantly worry about physical safety, financial stability, being respected for our business acumen, and being treated accordingly.”
Health Connect organizes calendars and tracks appointments that ensure timeliness and user safety. “A woman entering an unknown private residence for the first time faces a much higher risk than a man,” she observes. “We want to ensure that trust runs in both directions. The health professional is safe and feels safe to provide quality services, while the customer is assured of receiving that service.”
Overcoming gender challenges to support women-led innovation and entrepreneurship requires acknowledging that women are a unique asset. In Africa, where over 70 percent of health professionals are women, process innovation without significant involvement of women in design, implementation, and policy leadership is counterproductive. Women entrepreneurs typically face not just enormous financing challenges but also gender-related hurdles at every stage including social and cultural expectations that they should be homemakers and mothers first. Adverse social norms are not unique to Africa. In South Asia, it is not uncommon for women to leave the workforce after marriage. In many Pacific island countries, women often bear the financial commitments of their extended family.
Women-led solutions in Africa such as Health Connect can be models for addressing similar situations in other regions including the Asia Pacific. The key lesson: The various players that can make these innovations a reality – the technologists, the designers, the policy makers, the financiers, and the implementers – have to understand the often very obvious obstacles that are preventing women – the most underutilized talent pool in many countries – from fully contributing to driving on-the-ground scalable innovations in healthcare, a field where females are already well represented. Recognizing these hurdles and taking them into account when designing processes, services, regulations and policy will unlock the full potential that women in healthcare offer.
Further reading:
Check out here for more research and analysis from Asian perspectives.