A one-size-fits-all approach to containing the coronavirus pandemic such as the imposition of blanket lockdowns does not work for any nation. Instead, argues Bryane Michael of The University of Hong Kong, health authorities must adopt a targeted approach so that different populations or population segments are treated differently based on their relative risk assessment.
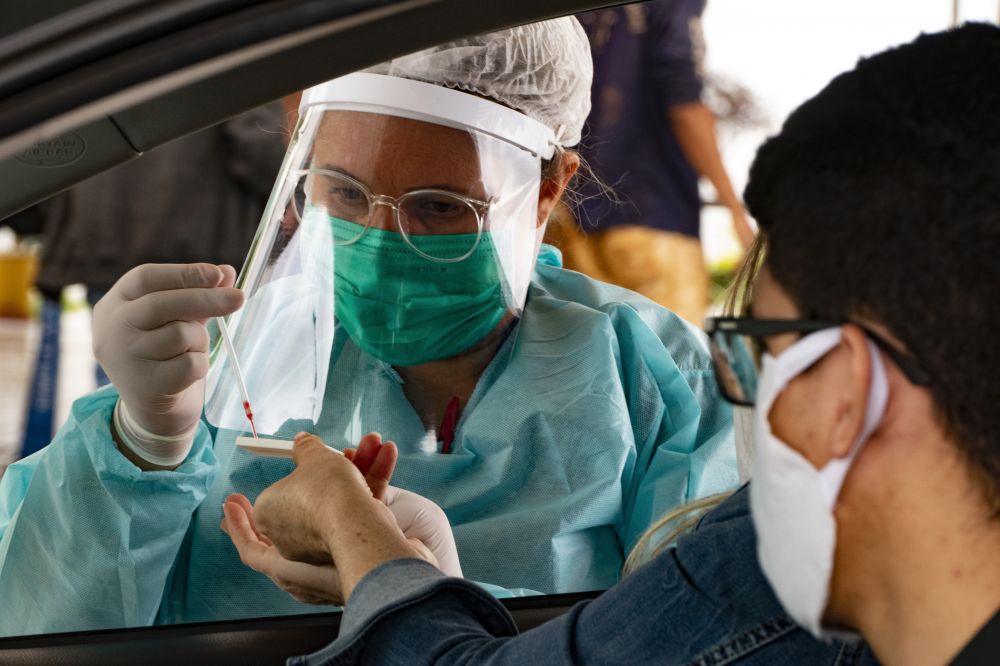
Drive-though coronavirus testing in Águas Claras, Brazil: A targeted risk-based approach to the pandemic would be more effective than a blanket strategy such as a lockdown (Credit: Leopoldo Silva/Agência Senado)
When the coronavirus crisis emerged, governments around the world first under-reacted, then over-reacted. In other words, they ignored a raft of law and policy advice developed since the 1960s to deal with pandemics and other forms of social risks. They even ignored plans already made to adopt measures proposed by the World Health Organization (WHO) in consultation with health authorities in member states.
Why reinvent the wheel?
Since roughly the end of World War II, government policymakers have adopted risk management methods across the board. From the UK’s environmental policies to the whole-of-government approach, official policy has prioritized risk management with risk-based policies. In this view, best practice in a range of fields, especially and including the management of pandemics, entailed treating different populations differently.
The current universal and indiscriminate shelter-in-place policies represent the most odious, harmful and unnecessary part of the policy response to the Covid-19 crisis. Not only because of the economic and social harm they have caused, but particularly compared with an alternative risk-based approach. No one argues for eliminating all lockdowns, as many obviously save lives. But such lockdowns should be done by on a localized risk-based basis.
The law and the public clearly recognize what executive bodies across the world have not. From Oregon and Wisconsin in the US to Malawi, courts have struck down one-size-fits-all quarantine policies. Even before considering issues such as legal rights, our laws have embodied the risk-return trade-off. Yet, places like Bosnia still do not get it and they confuse risk-profiling with capricious discrimination.
No population has unquestioningly accepted lockdowns and other strong measures. Each individual knows the risk factors most pertinent to his or her local conditions far better than any jurisdiction-wide rule could cover, even though ignoring these rules may be illegal and the application of them often very, very wrong, or at least counter-productive. The SafeGraph graphic below shows such an approach already happens in practice whether policymakers like it or not. Why not use data to implement these rules better and with greater precision? In other words, find the places that are virus hot spots or highly vulnerable (potential clusters) such as nursing homes and focus lockdowns and other measures on those areas.
What would such risk-profiling look like?
The social sciences have much to teach us about managing a pandemic. Just as customs agents do not search every bag, health workers do not test everyone – they need to focus principally on risky people, places and things. Stratified random sampling accounting for risk represents the best way to allocate resources. Focus on high-risk groups such as those who came from Wuhan in the early days of the outbreak. Focus on the pockets of the sick and work your way back using increasingly better methods of sampling social networks.
A risk-based approach would seem to “over-test”. Why give healthy people tests? The UK recommended testing for people who had (or thought they had) symptoms. The Americans seemed to pursue a smarter strategy by urging that symptomatic patients not be tested. Instead, you want to test every group in proportion to its riskiness. A well-functioning, risk-based testing regime would show a lot of negative results, not just a few. No surprise that, as shown in the chart below, New Zealand represents one of the best examples of this philosophy. Like throwing darts, you close in on the target parameter and reduce testing in groups that show a lot of negative results, keeping test reliability and other relevant issues in mind.
Revenge of the “risk society”
In practice, risk-based testing and policies face a host of political and social problems. After all, if a black or minority population has a higher incidence of infection, would focusing on them be racist? Lack of empirical data leads to political, social or sometimes just inexplicable discrimination. Many countries and people feared Asians at the start of the crisis because an Asian origin was the only inference available. Without data, the only recourse was one-size-fits all policies. Everyone gets their temperature taken, not just Asians.
Some see more nefarious, or at least negligent, intentions behind one-size-fits-all quarantines, face-mask wearing and other measures applied indiscriminately across an entire jurisdiction. The Covid-19 crisis brings to mind the concept of the risk society, which sociologists Ulrich Beck and Anthony Giddens described as the way in which a modern community responds to risk, with a limited group of influential people deciding the allocation of risk’s costs. Usually, those blanket policies have “asymmetric costs” such as senior policymakers and other privileged persons still collecting a paycheck, while small business owners do not.
The widespread decision not to use risk-based means of testing and treating Covid-19 outbreaks points to the incentives driving our risk society. Necessarily existing polices do not pave the way for an ever-expanding state control over our lives. Yet, the US’s failure to rope in millions of unemployed to fight the crisis – rather than just subsidize millions at home – does have very real economic impacts and implications. Providing social protection through digital payments can seem heartless, given that many middle-class people or those who eschew e-banking or citizens that live abroad do not use these platforms or are unable to access them.
The need for targeted risk-based solutions
No doctor treats a patient before he or she administers tests. Yet billions of patients underwent the indiscriminate social treatment of a lockdown before any testing. Much of the data accumulated and analyzed during this pandemic consisted of hearsay and post-infection hospital visits, which is hardly a healthy basis for establishing risk baselines.
The risk-society approach will remain. Yet only by quantifying the risks through risk-based testing and then applying risk-based treatment can we hope to avoid the unintentional side effects of our coronavirus policies.
Check out here for more research and analysis from Asian perspectives.